March 05, 2026
The Hidden Importance of Baby Teeth for Your Child’s HealthDiscover why baby teeth are crucial for your child’s oral development, speech, and overall health. Learn tips for care and early prevention of dental issues.
March 05, 2026
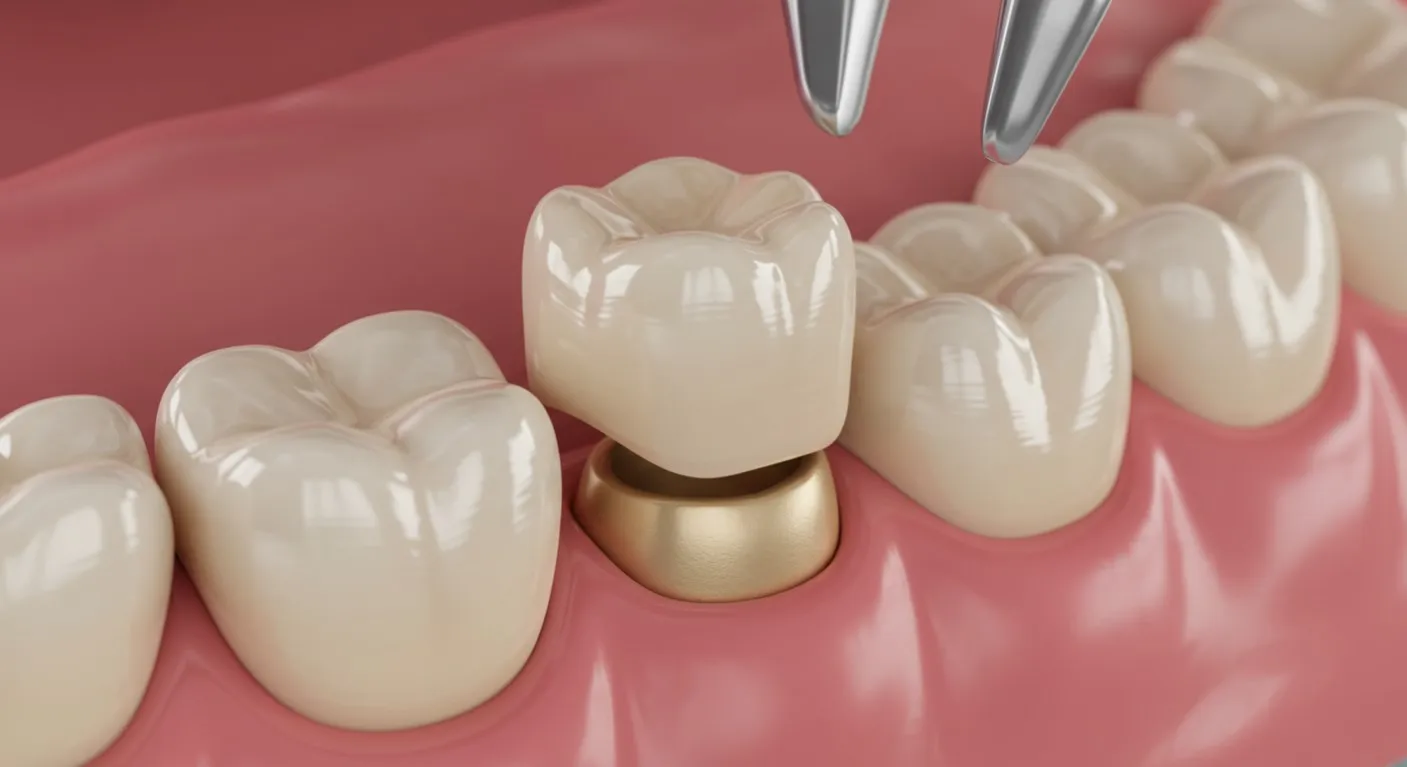
A dental crown is one of the most trusted and effective restorations used in modern dentistry. It functions as a protective cap that completely covers a damaged, weakened, or misshapen tooth. By restoring its original strength, size, and appearance, a crown not only enhances the smile but also allows normal chewing and speaking.
Dental Crowns can be made from porcelain, ceramic, zirconia, metal alloys, or porcelain fused to metal each material chosen to match your needs in durability and aesthetics. Dentists often recommend crowns for teeth that have been treated with root canals, suffered large cavities, or fractured under pressure.
There’s a widespread belief that once a crown is placed, the tooth beneath it becomes invincible safe from all future decay. After all, the crown covers the entire tooth surface. But while a crown provides strong external protection, the tooth underneath is still very much alive and vulnerable to bacterial attack.
Yes it absolutely can. The crown itself is artificial, so it won’t decay, but the natural tooth beneath and around the edges can still develop cavities if bacteria find their way in. In fact, decay under a crown is one of the leading causes of crown failure and tooth loss if not caught early. Let’s explore how this happens and what you can do to prevent it.
Even though a dental crown covers most of your tooth, it still relies on a healthy foundation. Cavities under crowns usually start small and hidden, often forming near the crown margins the tiny space where the crown meets your gumline.
When a crown is placed, the dentist cements it securely to seal out bacteria. However, over time, the seal can wear down due to chewing forces, temperature changes, or natural cement erosion. Once bacteria slip into this space, decay begins silently under the crown.
Plaque a sticky biofilm of bacteria forms on all tooth surfaces, including around crowns. If not removed daily through brushing and flossing, the bacteria in plaque release acids that erode the underlying tooth. The decay can spread beneath the crown, weakening the natural tooth and threatening its nerve.
Because the crown hides most of the tooth, you can’t see or feel the decay until it becomes severe. Many patients assume their tooth is fine because the crown looks intact. Unfortunately, by the time pain appears, the cavity may already have reached the inner layers of the tooth.
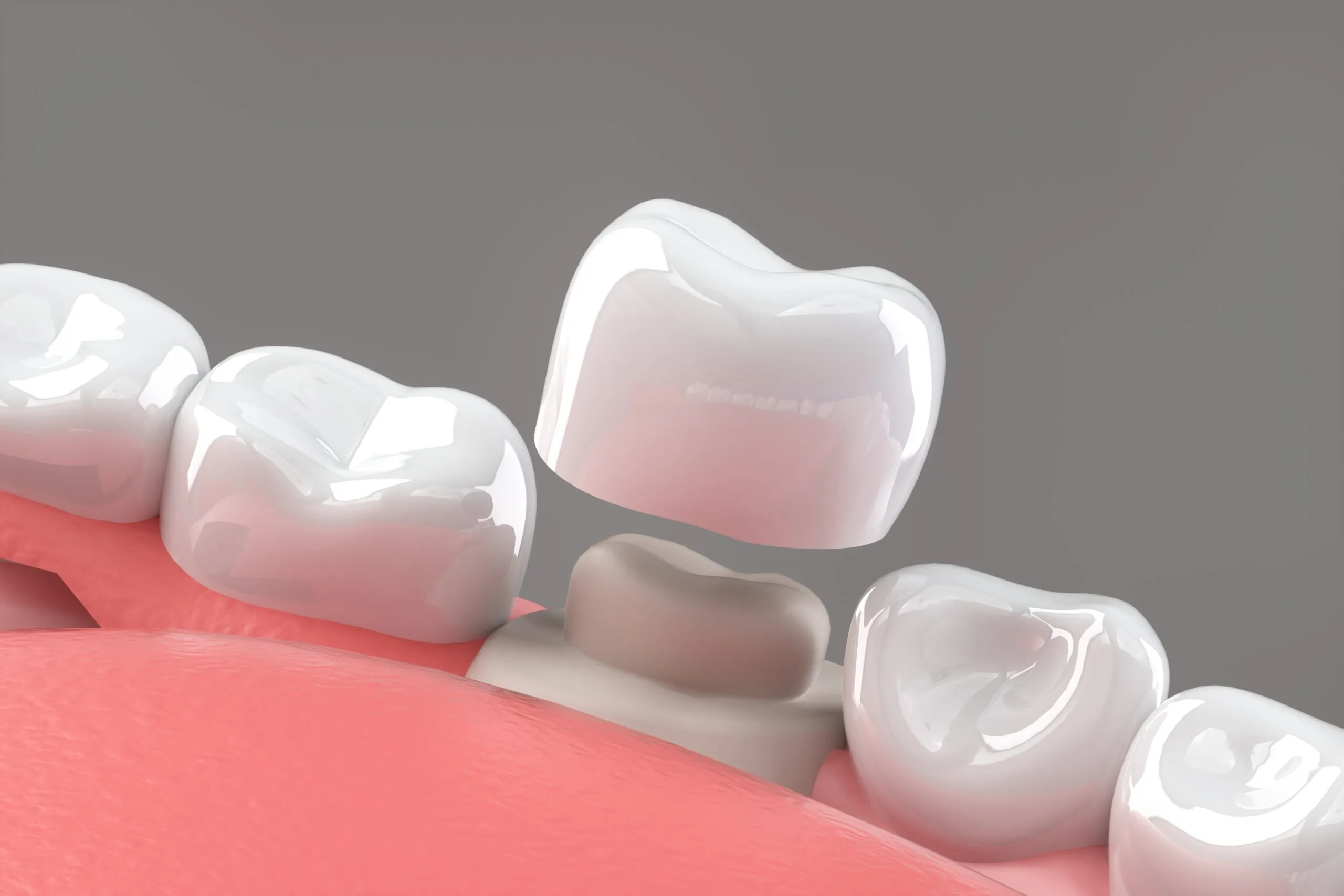
While any crowned tooth can develop decay, certain conditions make it more likely. Understanding these causes helps you take preventive action before problems begin.
Failing to brush and floss regularly is the most common reason cavities form under crowns. Food particles and plaque can easily collect along the crown’s edges. If plaque isn’t removed, bacteria multiply rapidly, producing acids that sneak under the crown and attack the tooth.
Cement, though strong, isn’t indestructible. Over time, it can break down, especially under stress from chewing or grinding. Even a tiny gap along the crown margin provides the perfect hiding spot for bacteria. Once inside, decay can progress quickly beneath the crown.
As gums recede often due to age, aggressive brushing, or gum disease more of the tooth root becomes exposed. Since roots lack enamel, they’re highly prone to decay. If a crown’s edge becomes exposed because of gum recession, bacteria can attack that vulnerable area.
A diet high in sugary foods, sodas, and acidic beverages fuels bacteria that cause cavities. Acids soften the tooth surface and weaken the protective seal between the crown and tooth, creating conditions where decay thrives. Constant snacking or sipping sugary drinks can make this problem worse.
Bruxism grinding or clenching your teeth can loosen or crack a crown. When that happens, the cement seal may break, allowing bacteria to enter. Grinding also places extra pressure on the gumline, contributing to gum recession and increased decay risk.
If a crown wasn’t fitted precisely, small spaces may have been left between the tooth and the crown. These gaps are difficult to clean and easily trap bacteria. Likewise, old crowns that have worn down or shifted with time often develop leakage, making decay almost inevitable unless replaced.
Cavities under crowns rarely show clear signs early on. Still, there are several symptoms that can warn you something is wrong.
If you feel sudden sensitivity when eating hot, cold, or sweet foods, it may indicate that decay has reached the underlying tooth structure. This happens because the protective barrier of dentin is exposed to temperature changes.
Pain while chewing or a dull, throbbing ache around a crowned tooth can signal decay or infection beneath. Sometimes, the pain may come and go, making it easy to dismiss until it becomes severe.
Inflamed, red, or swollen gums around a crown often mean bacteria are irritating the surrounding tissue. If the gums bleed when you brush or floss near the crown, that’s a red flag that decay or plaque buildup is occurring below the surface.
Discoloration near the edges of the crown especially a dark shadow or line may indicate decay spreading underneath. This is one of the few visible signs of a cavity forming under a crown.
A loose crown is never normal. It usually means that decay has weakened the tooth underneath or the dental cement has failed. If you feel movement when biting or notice the crown lifting slightly, visit your dentist immediately.
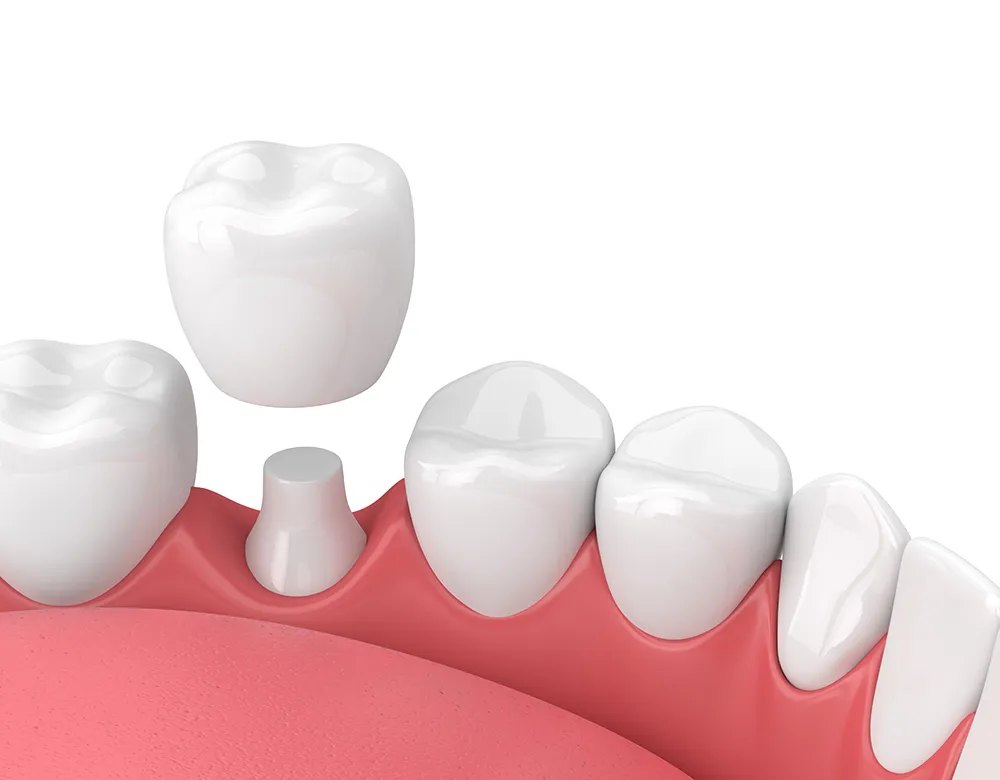
Dentists use several methods to diagnose hidden decay under crowns often combining technology and clinical experience for accuracy.
During a checkup, your dentist carefully inspects the crown margins for gaps, discoloration, or gum irritation. They might use a fine dental explorer to feel for soft spots or areas where the crown margin isn’t sealed tightly.
X-rays (bitewing or periapical) are the most effective way to detect decay beneath crowns. On an X-ray, decayed areas appear darker than healthy tooth structure, allowing the dentist to spot hidden problems early.
Modern clinics may also use digital scanners or laser fluorescence tools that can detect subtle changes in the tooth structure. These advanced methods help catch decay even before it becomes visible or painful.
Catching decay under a crown early can mean the difference between a simple repair and a complex procedure. Once decay spreads deep into the tooth, it can compromise the entire restoration, leading to root canal treatment or extraction.
The best treatment depends on how far the decay has progressed and how much of the tooth remains healthy.
If the decay is confined beneath the crown, your dentist will remove the existing crown, clean out all decay, and rebuild the tooth using filling material. Once the tooth is stable and healthy, a new crown is fabricated and cemented securely in place.
When decay has reached the pulp (nerve) of the tooth, root canal treatment becomes necessary. The dentist removes the infected tissue, disinfects the canals, and seals them with a durable material before placing a new crown. This treatment saves the natural tooth and eliminates pain.
In severe cases where the tooth structure is too damaged to support a new crown, extraction might be the only option. After removal, the missing tooth can be replaced with a dental implant, bridge, or partial denture to restore function and aesthetics.
If gum recession or gum disease contributed to the decay, your dentist may also recommend scaling, root planing, or soft tissue treatments to restore gum health before placing a new restoration.
The good news is that cavities beneath crowns are largely preventable with consistent oral hygiene and regular professional care.
Use a soft-bristled toothbrush and fluoride toothpaste to clean all surfaces of your teeth, especially around the gumline where plaque tends to build up near crowns. Electric toothbrushes are particularly effective for reaching tight spaces.
A daily rinse with antibacterial or fluoride mouthwash helps reduce harmful bacteria and strengthens tooth enamel. This step is especially important if you have multiple crowns or bridges.
Limit sugary snacks, carbonated drinks, and acidic foods that encourage bacterial growth. Drink water after meals to rinse away acids and maintain saliva flow, which helps neutralize bacteria.
If you suffer from bruxism, wearing a custom night guard can prevent damage to crowns and reduce pressure that leads to loose margins or cracks.
Visit your dentist every six months for cleaning and examination. Professional cleanings remove hardened plaque (tartar) that brushing alone can’t remove, while checkups help identify crown issues early before decay develops.
Don’t wait for pain or visible damage to take action. If your crown feels loose, looks discolored, or has visible cracks, have it checked and replaced before bacteria cause deeper problems.
Dental crowns are a fantastic way to strengthen and restore damaged teeth, but they’re not immune to future problems. The natural tooth beneath can still decay if bacteria infiltrate through small gaps or if oral hygiene slips. Recognizing early warning signs like sensitivity, gum irritation, or dark lines can help you act quickly before serious damage occurs.
The key to preventing decay under crowns lies in daily care and regular dental visits. Brush, floss, and rinse consistently, maintain a balanced diet, and never ignore discomfort around a crowned tooth.

March 05, 2026
The Hidden Importance of Baby Teeth for Your Child’s HealthDiscover why baby teeth are crucial for your child’s oral development, speech, and overall health. Learn tips for care and early prevention of dental issues.

March 05, 2026
From Sharp to Dull: What Different Tooth Pains MeanLearn what different types of tooth pain sharp, dull, or throbbing can indicate about your dental health and when to seek professional care.